The biggest concern with genital herpes during pregnancy is that you might transmit it to your baby during labor and delivery. Newborn herpes is relatively rare (about 1,500 newborns are affected each year), but the disease can be devastating, so it’s important to learn how to reduce your baby’s risk of becoming infected. You can transmit herpes to your baby during labor and delivery if you’re contagious, or “shedding virus,” at that time. The risk of transmission is high if you get herpes for the first time (a primary infection) late in your pregnancy.
Much less commonly, you can transmit the virus if you’re having a recurrent infection. If you’ve ever had a herpes outbreak, the virus remains in your body and can become reactivated. In rare cases, a pregnant woman may transmit the infection to her baby through the placenta if she gets herpes for the first time in her first trimester. If a baby is infected this way, the virus can cause a miscarriage or serious birth defects.
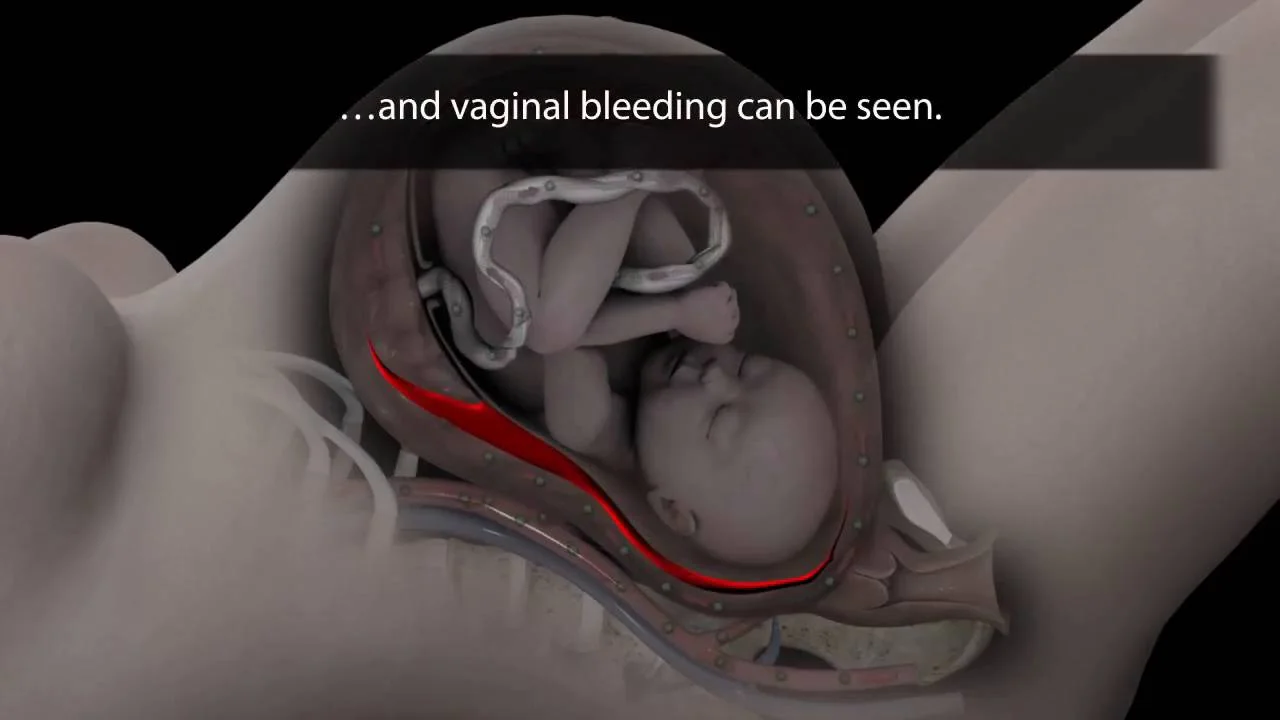
If you’re having an outbreak or symptoms of an impending outbreak when your water breaks or when you go into labor, you’ll need an immediate cesarean delivery. This would be the case if you have any visible sores on your cervix, vagina, or external genitals, or any symptoms, like tingling, burning, or pain, that sometimes signal an imminent outbreak. (Currently, there’s no quick and reliable way to test whether you’re actually shedding virus.)
To improve your chances of being able to deliver vaginally, most experts — including the American College of Obstetricians and Gynecologists — recommend that pregnant women with recurrent genital herpes be offered oral antiviral medication from 36 weeks or so until delivery. Recent studies show that this reduces the risk of an outbreak at the time of labor.
If you first get genital herpes late in pregnancy and blood tests confirm you’ve never had it before, some experts recommend having a cesarean section even if you don’t have symptoms when you go into labor. About a third of the time, newborn herpes affects a baby’s skin, eyes, or mouth, but not his other organs. If that’s the case, he may have sores at delivery or develop them up to four weeks later. They typically turn up between 1 and 2 weeks of age.
Herpes lesions usually look like blisters and can appear anywhere on a baby’s body. They often appear where there has been a small break in the skin or any trauma — like where the hospital wristband was or where an electrode was placed on his head to monitor his heart rate during labor.
If your baby has herpes that’s limited to the skin, eyes, and mouth and gets prompt treatment with intravenous acyclovir, he’ll most likely do well. One study showed that more than 90 percent of babies with this form of herpes were developing normally when they were tested as 1-year-olds, although an infected baby can have serious recurrent outbreaks or long-term problems.
If not treated promptly, a baby who starts out with herpes limited to the skin, eyes, and mouth can go on to develop an even more serious form of herpes.
In another third of newborns who get herpes, the central nervous system is affected. This most often shows up at about 2 to 3 weeks of age with symptoms such as irritability, fever, lethargy, poor feeding, or seizures.
The remaining third of newborns get what’s called “disseminated herpes”. This involves multiple organs, often the lungs and liver. It typically shows up during the first week after birth. Babies with disseminated herpes may or may not have skin lesions. (If they don’t, diagnosing herpes as the source of the baby’s illness is tricky.)
These latter forms of herpes are very serious. Unfortunately, even with prompt treatment, a number of these babies will die, and many of the survivors will end up with serious long-term health and developmental problems.